On this page, you will find information about What to Expect regarding:
Swallow Study (modified barium swallow or videofluoroscopic swallow evaluation)
Gastric Emptying
Scope: EGD, Esophagogastroduodenoscopy
Barium Swallow/Upper GI
Swallow Study (modified barium swallow or videofluoroscopic swallow evaluation)
What to Expect, by Jesse S. (January 2015)
You will go into an xray room and she will sit in a chair next to the xray machine. Make sure to bring a bottle that your [little one] lo will take. They will put a certain amount of barium in the bottle with no thickener and feed her while they take x-rays of her swallowing. If they see penetration they will thicken it to nectar and repeat. If penetration on nectar they will go to Honey. They will then try solids in the same manner. A speech/feeding pathologist is the one who will do the feeding and an MD will be there to take the xrays. Its easy as long as your lo is calm enough to sit in the chair and be fed good luck! You will know then and there if there are any issues.
Usually if there is penetration on a “thin” aka regular formula/bm then they want to thicken one step up to see if that solves the penetration issue. Most swallow studies are done a) to see if there is any anatomical swallow issues, b) to see if there is any esophageal penetration with thin liquids and c) to see if thickening to nectar or honey solves the issue of penetration with thin liquids.
Gastric Emptying
What to Expect, by Traci R. (January 2015)
Plan on lots of entertaining her to keep get distracted. They usually have them eat the mixture laying totally flat (which my kids hated) and then you watch it all go through. (At least if I’m remembering it right. I could be confusing it with a swallow study?)
It’s fascinating to watch (I think it is!), but the kids are usually pretty upset about it all. Plan for a needy baby the rest of the day. If she bounces right back, then you’ll be pleasantly surprised instead of frustrated by the clingy-ness.
They will want to her to lay still. I had to hold mine down. Maybe take a sucker? If they get the testing fluid, it and it won’t jack up the test, it might distract her. That and a tablet with a show or game. Your phone, perhaps.
No doubt she’s going to be pissed, though!
Scope: EGD, Esophagogastroduodenoscopy
What to Expect, by Anke T. (August 2015) CLICK HERE FOR MORE NOTES
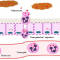
When it comes to procedures for diagnostic in GERD, a SCOPE is usually the first thing Gastroenterologists recommend and order. What it is exactly is something called an EGD, Esophagogastroduodenoscopy. As the name explains it already, the physician is using an endoscope to inspect visually the throat, esophagus, stomach and duodenum (the first part of the small intestine).
At the same time, s/he takes several biopsies of the tissues. In order to do this, there will be a certain amount of air pumped into the stomach, to avoid it sticking flat together. This procedure can only be done under general anesthesia; all possible risks are mostly coming from this. The air may cause some flatulence later, but should not be too bothersome.
Hospitals nowadays have a great routine in doing these EGD’s; they are performed way more often then 10 or 15 years ago, since reflux in infancy is on the rise, as are all these new EoE patients that pediatric gastroenterologist have to care for.
So you usually bring your child to the hospital at the time you have been told, go through the measuring and weighing process, and then into the prep room. Vital signs are taken, and the doctor and the anesthesiologist show up for a last conversation prior to the endoscopy. The child has a bed where it is assigned to, and wears a gown, diaper and hair net. The caregiver gets dressed in a gown-like disposable thing, on top of their regular clothes, dons a hairnet and shoe covers, too, in order to attend to the child all the way into the procedure room. Then the anesthesiologist places the mask on the little ones face, and Mom or Dad can give as much comfort as possible until the child is sedated. Then the caregiver needs to leave the room asap.
They will insert the IV once the child is under anesthesia, so they won’t feel the poke. The whole procedure takes 10 to 20 minutes and you meet your child in the recovery room, more or less miserable. Every time they are under General Anesthesia (GA) they tolerate it differently, and when the propofol is leaving their system sometimes they are not well at all. The chances for that are 30%. But as unpleasant this is, it is nothing harmful and usually fades away after 30 minutes. Still in the recovery room, the doctor shows up and hands out the report that also contains pictures, gives some brief information and usually recommends to have another appointment for a consultation, once the pathology report from the biopsies that were taken, is in his office. As soon as the vital signs are all checked and normal, IV removed, you can go home with discharge instructions.
A week later, you usually find yourself back in your Gastroenterologists office, ready for answers. And then, a lot of times there are nonr. Especially in infants under 8 months, the EGD may come back perfectly normal. Because there is no abnormality in anatomy, and no underlying condition that would cause any altercation in histologic findings. Under 12 months of age EoE can not be ruled out, if there are no eosinophils yet, they may still be to come. Sometimes the finding is EoE and then all the effort was worth it, because treatment should start imminently. But overall, for the GERD suffering child there may not be more coming out of it then a mildly inflamed esophagus, and this may be pretty obvious anyway, from the clinical appearance.
A hernia would be possible to diagnose, but more babies have none then one, and even if it is not seen it does not mean that there isn’t one. So overall it is questionable to me, if an EGD should always be the first thing to do, since it is quite invasive, and not really so beneficial every time. I even see more danger in the perfect result, because the whole affect of acid reflux takes some time of suffering; there is like a delay in time between suffering and visible damage, so Doctors would tend to underestimate the severity of GERD by an normal EGD. That does not mean the child is well, but they would present it that way. All of a sudden it is all Mom again, because the EGD was beautiful. No, that is not reality. My 7 month old son had a perfect EGD, I got an earful that it may all be behavioural until 13 months of age, then he had another EGD and it showed a hernia but still, only mild esophagitis. But I know that he was very symptomatic from that. But, at every doctors visit between 7 and 13 months I got rubbed in the face “but his EGD was normal”. If it wouldn’t have been for upper gastrointestinal bleeding and the FTT diagnosis at 13 months old, they would probably not have him scoped again.
Like I said, risks and benefits is somethig that carefully be calculated in every single case, not every child with reflux needs a standard protocol for diagnosing. An abdominal ultrasound should be the very first thing to do, since it is the least invasive and can rule out a lot of anatomy problems, especially in very young children when projectile vomitting is involved, and pyloric stenosis may be a possibility. Other then this, why not start with a 24 h pH probe? We know the child has reflux, let’s evaluate how bad it is. The important thing is, if it is the first pH probe ever done, insist on taking your child off any PPI for 7-10 days prior the test. Usually the doctor orders it that way, but some seriously want you to do it while ON. That is great to see whether or not if treatment is working, but for the first probe, we want to see how the reflux really is, unmasked.
This procedure is done in the endoscopy department of a childrens hospital, but does not have to be performed by a doctor; a special pediatric endoscopy nurse can do it. A small tube placed into the esophagus, through the nose. Not fun, but it can be done without general anesthesia. And once the tube is in place, the little ones don’t even mind it anymore, as long as they are left alone. Most of the times an x-ray is done, to confirm the tube is in the right place, and the attending hospital gastroenterologist is approving it. On the other end of the tube a device is connected, that records the pH levels and also shows them on a display. The tube will be taped and the device goes into a small pouch that can be attached to the clothes. Sometimes they want you to stay in the hospital. They may let you home.
The pH level in two places of the esophagus is measured and recorded for 24 hrs, distal and proximal by two spots in the tube. Distal is above the LES, proximal a little higher. You write a dairy, when your child ate, drank, slept. You also have a symptom button that needs to be pressed, whenever you think your LO is suffering an reflux episode. After the 24 h the tube can be taken out, totally pain free (if you are home you can do it yourself and only return the device), and the endoscopy department does the read out and the report goes back to the GI who ordered the study in the first place. As for the results, he gets a report that contains several pages. Some contain the graphs, with two variables, time and pH levels. One pages is a statistic of all the data collected. Total number of reflux episodes (pH < 4), total of time spend in pH levels under 4, and some interesting numbers like SCF the Symptom Correlation Factor – how many times you thought it was reflux and it actually was.
We had a symptom correlation of 98.8 for example, which left our Gastroenterologist baffled. Yes, we knew how he suffered and usually all parents do. So the pH study is a great way to get the whole misery into a written report. If you tell your doctor the reflux is bad, he is unable to comprehend. If he sees a report that shows “total number of reflux episodes in 24 h: 126”, then it is an information that he can process. Doctors somehow are that way. We had it done in our 14 month old son, he was a very active toddler by that time, but it was possible to have him home. I preferred it then being the hospital, but that depends on each parent, I can see if someone would be more comfortable in the hopsital.
So the overall conclusion, to me, is, why not always do the pH study first and then take it from there? Knowing how bad it really is will lead to proper medication and further testing. Another pH study while still ON PPI would also be a possibility to see if the PPI actually works, and covers the acid, if there is doubt. Depending on the results, there may be more diagnostics desired or not, and then an EGD could be helpful. So, the pH study confirms reflux, and the EGD is able to show causes or complications from it, not the reflux or evaluate the actual reflex. And since in a lot of cases it is a prolonged newborn reflux that will grow out, it needs to be managed and treated, the minority of cases has underlying conditions that must be detected with an EGD. But like I said, each case and child is a little different, so it always depends on the circumstances and symptoms. In general my opinion is “the scope” could be held off a while in favor of an 24 h pH study.
Last but not least, never agree to the barium swallow. This is so traumatic for babies, and the results are so unreliable (unless there shows up a hernia, but there is better diagnostic to find that) that is not worth it. A lot of radiation is involved. Chances are high that it does not show reflux, even if there is. My FTT child with upper gastrointestinal bleeding, esophagitis and a hiatal hernia had a perfect barium swallow study. No reflux or hernia present. The 24 h pH study one week later showed 126 reflux episodes in 24 h. In my theory, they get so stiff and cramped up from crying while under the x-ray machine, getting the barium fluid forced in, that it just does not show up their regular anatomie. I wish I would have not agreed to that, it was more harmful then anything. Especially since at a certain point you have to choose careful what you really allow your child to go through. They get psychological trauma eventually. My miserable child is now 19 months, has the fundoplication surgery done, and for the first time in his life he is off all medication and has no reflux. But we see the trauma, and so did his pediatrician, and he will start play therapy with a pediatric psychologist. But besides the barium swallow there is not much I regret. We had to go that way.
At the end of the day, it is YOUR child and you are the advocate. You know best. Do all the research you can, and always ask questions, it is important to be on top of it. You know the symptoms better then anyone, and you have the parental intuition. Nobody can replace that. And don’t agree to any medication, procedure, treatment, if you don’t think it is right. CLICK HERE FOR MORE ENDOSCOPY NOTES
Review article: proton pump inhibitor therapy for suspected eosinophilic oesophagitis
BACKGROUND:
Recent advances in eosinophilic oesophagitis (EoE) have confirmed the existence of a new disease phenotype, proton pump inhibitor (PPI)-responsive oesophageal eosinophilia (PPI-REE).
RESULTS:
Ten articles, including 258 patients with suspected EoE (152 children, 106 adults) undergoing clinico-histological re-evaluation after PPI therapy, were identified. In children, clinical response ranged from 78% to 86% on PPI.
CONCLUSIONS:
Symptom improvement is common with PPI therapy despite persistent eosinophilic infiltration.
Aliment Pharmacol Ther. 2013 Jun;37(12):1157-64.